Cancer Resection and Surgical Margins
After Robot Assisted Radical Prostatectomy
Surgical removal of the prostate is the gold standard treatment for localized disease. Radical prostatectomy offers the advantage of complete disease eradication plus precise staging and grading. With the anatomical dissection described by Walsh in the 1980’s, the functional and oncological outcomes have improved [2, 3]. To further reduce morbidity and improve convalescence, there has been increasing interest in minimally invasive treatments in oncology.
The primary goal of radical prostatectomy is complete removal of the cancer and hence no recurrence. Prostate cancer is unique because of the blood test PSA. One might ask if the prostate is removed why would you check the PSA? Well, if the prostate and all of the prostate cancer is removed there should be no detectable PSA. It is not uncommon for the PSA to read non-detectable for a period of time after surgery only to have the PSA levels elevate signaling a “PSA recurrence”. But for clarity sake what we mean by “PSA recurrence” is that not all of the cancer was removed at the time of surgery. The risk of not getting all of the cancer (recurrence) is associated with factors that are determined by the cancer such as aggressiveness and how long it has been growing. Parameters such as PSA level, stage and Gleason grade help us to try and “predict” the risk of prostate cancer recurrence. And clearly, if the cancer has been present long enough such that some of the cancer is outside of the field of surgical removal recurrence is inevitable no matter how thorough or complete the surgery. However, there are cases where the complete surgical removal was not as complete as possible. This situation is termed a positive surgical margin (+SM). Thus of the adverse prognostic predictors, only surgical margins are dependent on surgical technique. Indeed when the cancer is confined to the prostate, a +SM can be attributed to technical error in incorrectly resecting the prostate during surgery.
A positive surgical margin is ‘defined as tumor extending to the inked-surface or margin of the prostate’ and is determined by the pathologist. One can think of this situation as removing an orange where the peel is the capsule of the prostate and the fruit is the cancer. If we get the entire prostate out according to plan the peel will be intact. However if there is violation of the peel and some fruit is exposed, one would assume that some of the cancer has spilled out. Hence, after the prostate is given to the pathologist the prostate is inked (similar if one put ink all around the orange). When the pathologist looks under the microscope and if they see cancer with ink on it, the assumption is that cancer was potentially left behind. The term “potentially” is used as not all +SMs do recur. So either there was some technical error in assessing the presence of a +SM or there was not enough cancer left behind to survive or the patient’s immune system took care of the rest. Because this is all microscopic we don’t know for sure what happens, we just know that it happen with a moderate amount of frequency (nearly 50% of the time – see below). Under most circumstances the presence of one or more positive surgical margins is revealed when the pathology report returns a few days after surgery.
The risk of a +SM is dependent on how much cancer is present in the prostate gland and if it has encroached one of three areas: 1. the apex of the prostate, 2. laterally near the nerves for sexual function or 3. at the prostate base where the bladder connects to the prostate. Even with excellent technical skill some areas of the prostate are more prone to +SM. The area most prone to developing a +SM is the apex. There are reasons for this including the fact that cancer very commonly involves the apex and the apex of the prostate is sometimes “buried” deep underneath the pubic bone. This situation can be complicated a large vein which if the bleeding is not controlled well the surgeon is force to move along and the dissection loses precision.
A +SM at the base of the prostate is not as common as the apex primarily because cancer more commonly occurs in the apex as compared to the edge of the prostate base. Both the apex and base of the prostate do not have an obvious boundary, rather the connection is more of a blending. As one might expect, with experience and better technique +SMs occur less frequently. The posterolateral region is the site of the neurovascular bundle, and a region where critical nerves for erectile function are abutted. The surgeon must choose how close to the prostate to dissect to preserve the erectile outcomes, whilst not invoking a +SM.
Do Surgical Margins Matter?
Although the true impact of a +SM remains controversial, many authorities agree it is an independent poor prognostic indicator and results in higher PSA recurrence rates [4, 19-23]. In a multi-institutional study, Karakiewicz and associates reviewed the impact of +SM on 5,831 patients [24]. Positive surgical margins imparted a 3.7 fold greater risk of PSA progression, which continues through 10 years. Importantly, +SM increase the likelihood of PSA recurrence even in men with pT3a and pT3b stages. In another report the five-year PSA recurrence risk for +SM is between 42-64%, which is significantly higher than for similar patients with negative surgical margins -SM [22]. Swindle and associates reviewed their experience with 1389 RPs for clinical stage T1-T3 prostate cancer [4]. Their overall +SM rate was 12.9%, with 6.8% for T2 and 23% for T3. They demonstrated the 10 year PSA recurrence rate was 19% for –SM and 42% for +SM cases. The investigators concluded that a positive margin increased the risk of recurrence even after adjusting for concurrent risk factors (pretreatment PSA, Gleason grade, and stage). Others have demonstrated similar findings [23].
Optimal treatment of men with +SM remains uncertain, so the potential for surgeons to totally eliminate +SM is an attractive but elusive goal.
The Decline of Positive Surgical Margins over Time
Oncologic results from selected large contemporary open (retropubic and perineal) and standard laparoscopic radical prostatectomy series are listed in table I [25-31]. Positive margin rate ranged from 9%-24%. The largest series from Johns Hopkins, had 9035 RPs with 14.7% positive margins [24]. The selected laparoscopic series with over 1750 patients had 18.6%-21.1% positive margins.
Table I. Contemporary open and laparoscopic radical prostatectomy series: oncologic outcomes.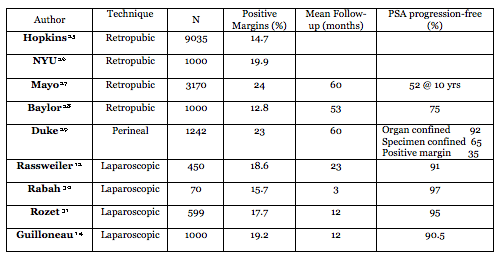
Table 2. Robot-Assisted Laparoscopic Prostatectomy Series: Oncologic Outcomes of studies with available pT2 and pT3 positive surgical margin rates. Percentages of pT2 to pT3 pathological cases for each institution, with the associated +SM rates.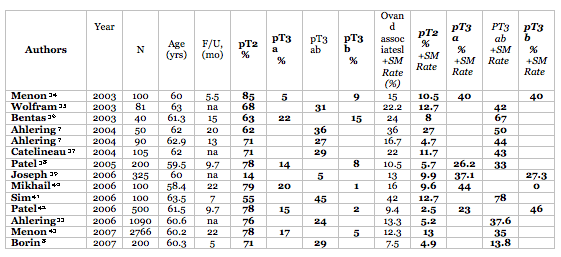
Technical Advances in Robotic-assisted Radical Prostatectomy
The robotic platform utilizes 10-12 x optical magnification in color, 3-D high-definition optics, a significant improvement over the limited magnification in open prostatectomy and 2-D optics of conventional laparoscopy. Blood loss is also significantly reduced, improving visualization of surgical planes.
New Techniques
In addition to technology advances and accumulated surgical experience, several technique refinements have been effective in reducing positive margins. Ahlering and co-workers described three important technical steps to aid in the apical dissection: 1. removal of all fat overlying the dorsal venous complex (DVC) and prostate, 2. full dissection of the levator fibers to expose and increase the DVC length, division of the puboprostatic ligaments, and 3. division of the DVC using a laparoscopic vascular stapler (Figure 1B). The overall +SM in their initial 50 cases when compared to their next 200 consecutive cases declined from 36% to 16.7%.
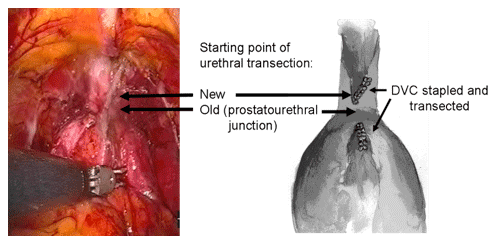
Subsequently in 2009, Ahlering’s group described a further modification to the apical dissection, which further reduced +SM. After careful clinical and pathological review the point of urethral transection was altered to include 3-6 mm more of urethra (Figure 2). Evaluation of the most recent 600 consecutive cases revealed the overall +SM rate declined to 7.5%. For tumors staged pT3/4 the +SM rate declined from 40% to 17.8%. For cancers confined to the prostate, pT2, the +SM has been reduced to 2%.
Figure 1.
First Technique to reduce positive margins.
Old Fat overlying the prostate was not removed
New The DVC is stapled and divided with an EndoGia stapler such that the apex and prostatourethral junction can be readily identified.
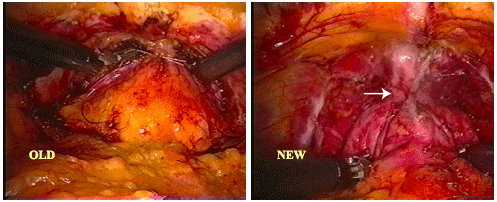
Figure 2.
Second Technique to reduce positive margins
Is there a Role for intra-operative Frozen Section to help reduce positive margins?
Intraoperative frozen section biopsy has been recommended in radical prostatectomy. The problem with most +SMs is that they are microscopic and hence the surgeon has no real feeling or worry of the presence of a +SM. Most surgeons will check a frozen section if they are concerned or unsure of how the tissue looks or feels. In this case the abnormal tissue is usually obvious.
So if the surgeon is concerned that there maybe residual tissue or cancer the frozen section is very useful in converting a possible +SM to a –SM [46]. However, routine use of frozen section on all cases to be “sure” of getting negative margins although enticing has not fulfilled its dream.
Figure 3a.
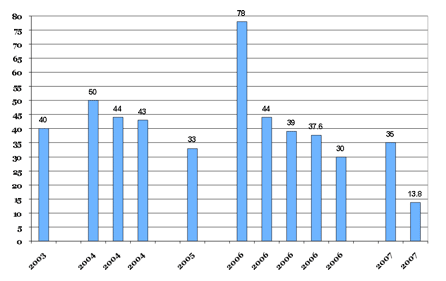
Reported rates of percent pT2 +SM rates in robotic-assisted prostatectomy for the years 2003-2007. 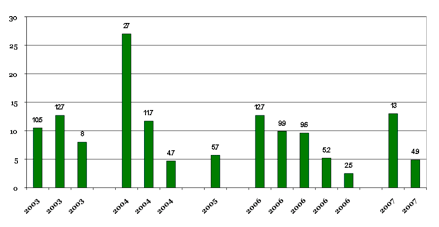
Figure 3b.
Reported rates of percent pT3 +SM in robotic-assisted prostatectomy for the years 2003-2007.