Sexual Function or Potency
After Robot Assisted Radical Prostatectomy
Importance of Evidence-based, Data-derived Potency Expectations
Sexual function is, for approximately 50% of men, one of the most troubling potential side effects of radical prostatectomy or any treatment of prostate cancer. Careful analysis of patient characteristics and surgical outcomes has highlighted a number of important factors that help predict your overall chance for recovery of potency. The most important factors that predict recoverability of sexual function are (younger) age and (normal) preoperative sexual function. For assessing “normalcy” of sexual function we use the International Index of Erectile Function abbreviated questionnaire (IIEF-5). You may also see the IIEF-5 termed SHIM (Sexual Health Inventory in Men). The IIEF-5 has been extensively studied and validated in the US, Europe and around the world. There are just 5 questions (see appendix) selected for ease and reproducibility. A normal score is 22-25. Mild dysfunction is 17-21. Moderate dysfunction is 12-16. Moderately severe dysfunction is 8-11 and severe dysfunction is 7 or less. As far as age is concerned the risk of sexual dysfunction increases with advancing age. Figure 1 demonstrates the percentage of men across decades with IIEF-5 of 22-25.
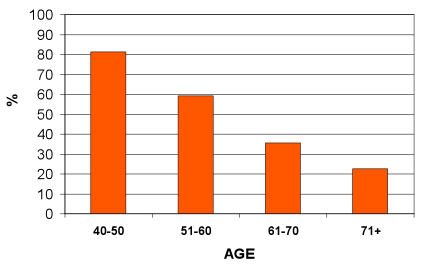
Beyond these patient-related factors are factors such as surgeon skill and experience. Additionally, assuming good surgeon skill there are physiologic factors that impact how long recovery takes from the surgery related trauma and inflammation. What does surgery related trauma or inflammation mean? Well experience has shown that the nerves in the NVBs are small and wiry like a strand of hair. They are very susceptible to stretch. As discussed above, younger healthy men tolerate the trauma better and recover quicker.
Although this constellation of variables differs for any given man, surgeons can make experience-based estimates based on analyses of their own data. When scrutinizing a surgeon’s potency outcomes it is logical that they should give data in their best case scenario. Why? Well a surgeon only has control over surgical skill and technique. So, if a surgeon has perfect skill and technique they generally will not preserve sexual function in a man with pre-existing erectile problems or dysfunction. This surgery is not going to make (partially) impotent men potent! Beware of surgeons who quote expected potency rates based on reports from the general literature, because those will not necessarily match what could (and should) be derived from their own evidence-based, data-derived outcomes.
Anatomy of Sexual Function
A major factor in your ability to achieve an erection is your “electrical hardware” - the nerves that carry signals that control the flow of blood into the penis, and control theretention of the erectile state. The erectile nerves are in reality an interwoven set of nerves and blood vessels, called neurovascular bundles (NVB), which can be thought of as a bundle of wires in an electrical circuit. The two neurovascular bundles run along the surface of each side of the prostate are intimately contained within a delicate layer of tissue called fascia.
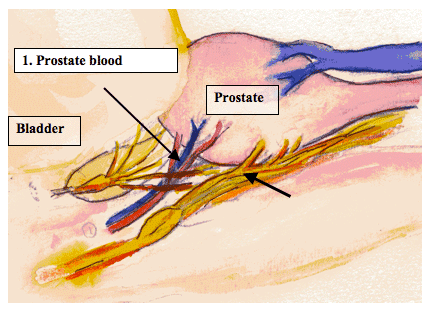
Depending on the pathologic features from your prostate biopsy, which may indicate an increased risk of whether cancer has likely spread outside the prostate (extraprostatic extension), your surgeon may recommend removing these nerves on one or both sides (i.e. wide excision) to maximize the chance of removing all of the cancer. If there is a no cancer outside the prostate, or a small amount of cancer on one or both sides, the surgeon may recommend “sparing” the nerves, which means that one or both bundles will be carefully separated from the prostate, so that they are left intact and not removed with the prostate. The amount of trauma endured by the neurovascular bundles during the nerve-sparing step is one factor which will determine the time required for the nerve to recover its erection-supporting electrical function.
Nerve-sparing Technique
A “nerve-sparing” procedure involves dissecting the nerve bundle off of the side of the prostate. This is one of the most delicate steps of your surgery. What once was a nebulous and difficult part of the procedure is now technically feasible and less traumatizing with the robot. While robotic-assistance does offer enhanced visualization of the neurovascular bundles and increased surgical precision, it does not make up for sloppy technique. Even with perfect technique, moving the nerves from their natural location on the side of the prostate will likely cause some nerve dysfunction or damage which can range from mild to severe. Our research has led us to several key findings to help minimize nerve injury: 1) thermal energy (cautery, heat) should be avoided or at least minimized, 2) nerve traction (stretching) should be avoided, and 3) dissection of the nerves causes inflammation which can be reduced with hypothermia (cooling) (Finley et al Urology, 2009; also for more detail, see Chapter 10 - Latest Advances).
In a recently published article, we analyzed the return of potency after robotic prostatectomy with unilateral wide excision of one neurovascular bundle compared with preservation of both neurovascular bundles (Finley BJU Int 2009). To study this issue we selected a cohort of men who were < 65 years and had “normal” preoperative sexual function. As shown in the following figure, for men who underwent unilateral nerve-sparing surgery (UNS), 80% regained potency at 24 months. For men who underwent bilateral nerve-sparing surgery (BNS), 93% regained potency at 24 months. It is evident from these curves that about half of these men regained potency between 9 and 15 months. These curves tend to shift downward with increasing age and impaired preoperative erectile function. This information serves to guide your expectation and understanding of how you may fare after surgery, keeping in mind the importance of other variables, such as prostate weight, that will affect the outcome.
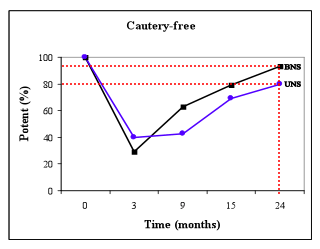
What to Expect
It is important for you to have credible expectations regarding your chance of recovering erections. Patients with pre-existing baseline erectile dysfunction can expect a significant decrease in post-operative sexual function, which is likely to be permanent. If you have good erections before surgery and you have a nerve-sparing procedure, you have a good chance of recovering function. However, expect that this may take months or years to occur. Immediately after surgery you most likely will not be able to achieve an erection. Your nerves will not be functioning, but will be disabled as if they were in a concussion-like state of shock, from which they will require months to recover. At the “happy end” of the bell-shaped curve of expected outcomes, approximately 5% of men will have erections within the first several post-operative weeks. About 30-40% will start having return of function at about 6 months, but as noted above this is variable and depends on a number of factors other than time (preoperative erectile function, age, nerve-sparing, prostate size etc).
Evidence is emerging that a daily low dose of Phosphodiesterase type 5 inhibitors (PDE5-Is) such as Viagra or Cialis (i.e. ¼ tab, 25 mg) before and after surgery can help improve recovery of erectile function (Mulhall JP 2008; Kovanecz I 2008; Vignozzi L 2006; Carson 2005). Think of this as a vitamin for your penis. These data show that this class of medications serves a protective role to the erectile nerves and to the penis by improving oxygen flow, promoting nerve regeneration, and preventing structural alterations such as fibrosis (scarring) and apoptosis (cell death), (Mulhall JP, 2008). In addition to this daily dose of PDE5-I, we encourage patients to utilize demand dosing – take a full dose of PDE5-I with sexual stimulation. Your initial erections, when they occur, will be soft and partial, however as you continue to recover they will become stronger and more full.
Penile Rehabilitation
The above medications represent just one component of “penile rehabilitation,” a program of recovery that is essentially physical therapy for the penis. Approaches to maximize the rehabilitation of erectile function after radical prostatectomy include chemical and physical means to produce an erection that not only produces pleasure, but rehabilitates erectile function by stimulating nerves and tissues, and flooding the region with oxygenated blood. Many men find these treatments successful and easy.
Chemical means. Drugs applied directly to the penis can deliver an erection by means of chemical effect on internal tissues. These include intracavernosal injection with prostaglandin E1, and urethral suppositories such as Muse.
Physical means. Vacuum pump devices create differential pressure to pull blood into the penis and thereby mechanically deliver an erection.
Aggressive intervention. Men need to understand that aggressive penile rehabilitation requires early intervention and chronic therapy, which in turn depends on the patient’s initiative.
Surgical Options. For those who do not regain erectile function after rehabilitative efforts, surgical options are available, such as an inflatable penile prosthesis.
Potency Results after Open Retropubic Radical Prostatectomy (RRP)
Much like continence, the definition of potency and standards of reporting are fraught with variability. Potency rates reported in the literature vary according to the author’s definition of potency, the methodology for data collection, the surgical technique, patient characteristics and the surgeon’s experience. For example, in the past, many studies consisted of surgeon-reported sexual outcomes rather than patient-reported. More recently, validated sexual health outcome survey instruments (questionnaires) have more accurately captured potency outcomes and quality of life parameters following surgery. When analyzing scientific articles or quoting potency rates, the statistician should calculate potency rates for cohorts of pre-potent men only (men capable of erection before surgery) and not cohorts containing both pre-potent and impotent individuals.
A review of data from the elite high volume academic surgeons serves as a reference point for what can be achieved with open surgery. Walsh reported that 69% of potent men who underwent unilateral nerve-sparing surgery (UNS) in his series were potent on long-term follow-up compared to 85% who underwent bilateral nerve-sparing surgery (BNS) (Walsh 1987).
In a seminal report, Catalona analyzed outcomes of 858 open radical prostatectomies and found that for pre-potent men with at least 18 months of follow-up, potency was recovered by 68% who underwent bilateral nerve-sparing and by 47% who were treated with unilateral nerve-sparing procedures (Catalona 1999). When stratified by age, among pre-potent patients in their 40s, 50s, 60s, and 70s who underwent a nerve-sparing procedure, potency was preserved in 90%, 80%, 60%, and 47% of men, respectively. In a subsequent paper, Catalona reported a similar trend in overall potency rates at 18 months, finding potency preservations of 53% and 76% after UNS and BNS open radical prostatectomy, respectively [Kundu & Catalona 2004].
In a recent prospective study of patients undergoing open radical prostatectomy by Eastham and Scardino at Memorial Sloan Kettering Hospital, patients completed questionnaires at home and were considered potent when they reported themselves able to have erections hard enough for penetration much more than half the time with or without PDE5-Is (Touijer K, 2008). Among pre-potent men, 96 of 164 (58.5%) were potent at 24 months post-operatively.
Lepor’s group reported a single surgeon series of more than 650 men undergoing open RRP with a minimum of 24 months follow-up (Marien 2009). Men were considered potent if they responded by validated questionnaire that they had engaged in sexual intercourse with only the use of PDE5I. Overall 59% of men (median age = 57 years) were potent at 24 month follow-up. Of men who underwent either a bilateral or unilateral nerve-sparing procedure, 61% and 47% were potent, respectively.
More sobering data, derived from the Prostate Cancer Outcomes Study (PCOS), which may be more representative of community hospitals rather than academic medical centers, found potency rates at 18 months of 41.4% after open UNS compared with 44% after BNS [Stanford et al 2000].
Potency Results after Robotic-Assisted Laparoscopic Prostatectomy (RARP)
Outcomes from robotic series are at least as good, if not better than those reported for open prostatectomy. Our data has shown that among preoperatively potent men aged less than 65 who underwent a nerve-sparing procedure, 89.7% were able to have satisfactory erections at 24 months.
Patel reported 78% of men were potent at 12 months following RARP (Table 1). Costello’s group reported on outcomes of 400 consecutive patients with a mean age of 60.2 years. From the overall population of 400 men, a cohort of 232 pre-potent men
